- 著者
- Koji Tamai Hidetomi Terai Akinobu Suzuki Hiroaki Nakamura Masaomi Yamashita Yawara Eguchi Shiro Imagama Kei Ando Kazuyoshi Kobayashi Morio Matsumoto Ken Ishii Tomohiro Hikata Shoji Seki Masaaki Aramomi Tetsuhiro Ishikawa Atsushi Kimura Hirokazu Inoue Gen Inoue Masayuki Miyagi Wataru Saito Kei Yamada Michio Hongo Kenji Endo Hidekazu Suzuki Atsushi Nakano Kazuyuki Watanabe Junichi Ohya Hirotaka Chikuda Yasuchika Aoki Masayuki Shimizu Toshimasa Futatsugi Keijiro Mukaiyama Masaichi Hasegawa Katsuhito Kiyasu Haku Iizuka Kotaro Nishida Kenichiro Kakutani Hideaki Nakajima Hideki Murakami Satoru Demura Satoshi Kato Katsuhito Yoshioka Takashi Namikawa Kei Watanabe Kazuyoshi Nakanishi Yukihiro Nakagawa Mitsunori Yoshimoto Hiroyasu Fujiwara Norihiro Nishida Masataka Sakane Masashi Yamazaki Takashi Kaito Takeo Furuya Sumihisa Orita Seiji Ohtori
- 出版者
- The Japanese Society for Spine Surgery and Related Research
- 雑誌
- Spine Surgery and Related Research (ISSN:2432261X)
- 巻号頁・発行日
- vol.1, no.4, pp.179-184, 2017-10-20 (Released:2017-11-27)
- 参考文献数
- 26
- 被引用文献数
- 3 3
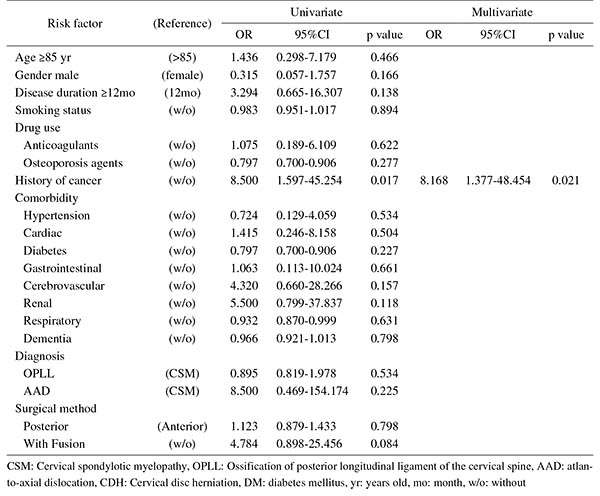
Introduction: With an aging population, the proportion of patients aged ≥80 years requiring cervical surgery is increasing. Surgeons are concerned with the high incidence of complications in this population, because "age" itself has been reported as a strong risk factor for complications. However, it is still unknown which factors represent higher risk among these elderly patients. Therefore, this study was conducted to identify the risk factors related to surgical complications specific to elderly patients by analyzing the registry data of patients aged ≥80 years who underwent cervical surgery.Methods: We retrospectively studied multicenter collected registry data using multivariate analysis. Sixty-six patients aged ≥80 years who underwent cervical surgery and were followed up for more than one year were included in this study. Preoperative patient demographic data, including comorbidities and postoperative complications, were collected from multicenter registry data. Complications were considered as major if they required invasive intervention, caused prolonged morbidity, or resulted in prolongation of hospital stay. Logistic regression analysis was performed to analyze the risk factors for complications. A p-value of <0.05 was considered as statistically significant.Results: The total number of patients with complications was 21 (31.8%), with seven major (10.6%) and 14 minor (21.2%) complications. Multivariate logistic regression analysis, after adjusting for age, revealed two significant risk factors: preoperative cerebrovascular disorders (OR, 6.337; p=0.043) for overall complications and cancer history (OR, 8.168; p=0.021) for major complications. Age, presence of diabetes mellitus, and diagnosis were not significant predictive factors for complications in this study.Conclusions: Preoperative cerebrovascular disorders and cancer history were risk factors for complications after cervical surgery in patients over 80 years old. Surgeons should pay attention to these specific risk factors before performing cervical surgery in elderly patients.
- 著者
- Seiji Ohtori Masayuki Miyagi Gen Inoue
- 出版者
- The Japanese Society for Spine Surgery and Related Research
- 雑誌
- Spine Surgery and Related Research (ISSN:2432261X)
- 巻号頁・発行日
- vol.2, no.1, pp.11-17, 2018-01-20 (Released:2018-01-27)
- 参考文献数
- 91
- 被引用文献数
- 41
Introduction: Many patients suffer from discogenic low back pain. However, the mechanisms, diagnosistic strategy, and treatment of discogenic low back pain all remain controversial. The purpose of this paper was to review the pathological mechanisms of discogenic low back pain.Methods: Many authors have investigated the pathological mechanisms of discogenic low back pain using animal models and examining human patients. Central to most investigations is understanding the innervation and instabilities of diseased intervertebral discs and the role of inflammatory mediators. We discuss three pathological mechanisms of discogenic low back pain: innervation, inflammation, and mechanical hypermobility of the intervertebral disc.Results: Sensory nerve fibers include C-fibers and A delta-fibers, which relay pain signals from the innervated outer layers of the intervertebral disc under normal conditions. However, ingrowth of these sensory nerve fibers into the inner layers of intervertebral disc occurs under disease conditions. Levels of neurotrophic factors and some cytokines are significantly higher in diseased discs than in normal discs. Stablization of the segmental hypermobility, which can be induced by intervertebral disc degeneration, suppresses inflammation and prevents sensitization of sensory nerve fibers innervating the disc.Conclusions: Pathological mechanisms of discogenic low back pain include sensory nerve ingrowth into inner layers of the intervertebral disc, upregulation of neurotrophic factors and cytokines, and instability. Inhibition of these mechanisms is important in the treatment of discogenic low back pain.
- 著者
- Shoichiro Takei Masayuki Miyagi Wataru Saito Takayuki Imura Gen Inoue Toshiyuki Nakazawa Eiki Shirasawa Kentaro Uchida Tsutomu Akazawa Naonobu Takahira Masashi Takaso
- 出版者
- The Japanese Society for Spine Surgery and Related Research
- 雑誌
- Spine Surgery and Related Research (ISSN:2432261X)
- 巻号頁・発行日
- vol.2, no.4, pp.294-298, 2018-10-26 (Released:2018-10-27)
- 参考文献数
- 22
- 被引用文献数
- 2 9
Introduction: Patients with spinal muscular atrophy (SMA) usually have progressive scoliosis. Although fusion of the sacrum or pelvis has been recommended for correcting pelvic obliquity (PO), the procedure is invasive. This study determined as to whether performing instrumentation to the fifth lumbar vertebra (L5) is safe and effective for scoliosis in patients with SMA.Methods: Twelve patients with SMA underwent posterior spinal fusion and stopping instrumentation at the L5 level. We evaluated age at surgery, the duration of surgery, blood loss, complications, preoperative and postoperative Cobb angles, and PO.Results: The mean age at surgery was 11.4 years; the mean duration of surgery was 319 minutes, and the mean blood loss was 1170 mL. The Cobb angle improved from 97.3° to 39.1° at 1 month postoperatively (correction rate, 60.9%) and to 42.3° at the final follow-up. PO was corrected from 27.8° to 13.1° at 1 month postoperatively (correction rate, 51.7%) and to 19.8° at the final follow-up. No complications were reported. All patients showed improvement in low back pain, with reduced difficulty while sitting. However, >10% correction loss of PO was observed in 6 patients with high preoperative PO.Conclusions: The correction rate of scoliosis in SMA patients with posterior spinal fusion and instrumentation to the L5 level was acceptable, and no complications occurred. Scoliosis associated with SMA was more rigid and severer than scoliosis associated with Duchenne muscular dystrophy. Correction rates of the Cobb angle and PO in SMA patients with instrumentation to L5 were similar to those in SMA patients with instrumentation to the sacrum or pelvis. Correction loss of PO was greater in patients with high preoperative PO than in those with low preoperative PO. Instrumentation and fusion to L5 for scoliosis in patients with SMA seems safe and effective, except in cases of high preoperative PO.