91 0 0 0 OA Rupture of Vertebral Artery Dissecting Aneurysm after mRNA Anti-COVID-19 Vaccination: A Report of Two Cases
- 著者
- Kohei CHIDA Tatsuhiko TAKAHASHI Suguru IGARASHI Kentaro FUJIMOTO Yasushi OGASAWARA Shunrou FUJIWARA Takahiro KOJI Yoshitaka KUBO Kuniaki OGASAWARA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.9, pp.95-100, 2022-12-31 (Released:2022-04-28)
- 参考文献数
- 19
- 被引用文献数
- 3
The coronavirus disease 2019 (COVID-19) pandemic continues to spread around the world, and widespread vaccination is considered the most effective way to end it. Although the efficacy of COVID-19 vaccines has been confirmed, their safety remains a concern. In this paper, we report two cases of ruptured vertebral artery dissecting aneurysm (VADA) immediately after messenger RNA (mRNA) anti-COVID-19 vaccination. In Case 1, a 60-year-old woman experienced sudden headache 3 weeks before her first dose of the Moderna mRNA-1273 COVID-19 vaccine. Magnetic resonance imaging showed dilatation of the right vertebral artery (VA) without intracranial hemorrhage. A day after the vaccination, she developed subarachnoid hemorrhage with pulmonary effusion due to a ruptured right VADA. She underwent endovascular internal trapping and parent artery occlusion under general anesthesia. In Case 2, a 72-year-old woman with a previous history of the left VA occlusion due to arterial dissection developed subarachnoid hemorrhage 7 days after the first dose of the Pfizer-BioNTech BNT162b2 COVID-19 mRNA vaccine due to a ruptured right VADA and underwent stent-assisted coil embolization under general anesthesia. The postoperative courses of these two cases were uneventful. The accumulation of more cases and further study are warranted to clarify the relationship between COVID-19 mRNA vaccination and ruptured intracranial dissecting aneurysms.
- 著者
- Yutaka MITSUHASHI Koji HAYASAKI Taichiro KAWAKAMI Takashi NAGATA Yuta KANESHIRO Ryoko UMABA Kenji OHATA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- vol.56, no.6, pp.326-339, 2016 (Released:2016-06-15)
- 参考文献数
- 75
- 被引用文献数
- 13 27
The cavernous sinus (CS) is one of the cranial dural venous sinuses. It differs from other dural sinuses due to its many afferent and efferent venous connections with adjacent structures. It is important to know well about its complex venous anatomy to conduct safe and effective endovascular interventions for the CS. Thus, we reviewed previous literatures concerning the morphological and functional venous anatomy and the embryology of the CS. The CS is a complex of venous channels from embryologically different origins. These venous channels have more or less retained their distinct original roles of venous drainage, even after alterations through the embryological developmental process, and can be categorized into three longitudinal venous axes based on their topological and functional features. Venous channels medial to the internal carotid artery “medial venous axis” carry venous drainage from the skull base, chondrocranium and the hypophysis, with no direct participation in cerebral drainage. Venous channels lateral to the cranial nerves “lateral venous axis” are exclusively for cerebral venous drainage. Venous channels between the internal carotid artery and cranial nerves “intermediate venous axis” contribute to all the venous drainage from adjacent structures, directly from the orbit and membranous skull, indirectly through medial and lateral venous axes from the chondrocranium, the hypophysis, and the brain. This concept of longitudinal venous axes in the CS may be useful during endovascular interventions for the CS considering our better understandings of its functions in venous drainage.
- 著者
- Shinichi YOSHIMURA Kazutaka UCHIDA Nobuyuki SAKAI Hiroshi YAMAGAMI Manabu INOUE Kazunori TOYODA Yuji MATSUMARU Yasushi MATSUMOTO Kazumi KIMURA Reiichi ISHIKURA Takeshi MORIMOTO
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- pp.rc.2021-0311, (Released:2021-12-24)
- 参考文献数
- 19
- 被引用文献数
- 13
Endovascular therapy is strongly recommended for acute cerebral large vessel occlusion (LVO) with an Alberta stroke program early computed tomography score (ASPECTS) ≥6 due to occlusion of the internal carotid artery or M1 segment of the middle cerebral artery. However, the effect of endovascular therapy for patients with a large ischemic core with an ASPECTS ≤5 (0–5) was not established. A multicenter, randomized, open-label, parallel-group trial was conducted to investigate the superiority of endovascular therapy over medical therapy without endovascular therapy for a large ischemic core with ASPECTS (3–5). Patients were randomly assigned to receive endovascular therapy or without endovascular therapy at a ratio of 1:1. The primary outcome was a moderate functional outcome, defined as a modified Rankin scale (mRS; scores ranging from 0 [no symptoms] to 6 [death]) ≤3 after 90 days. The secondary outcomes were defined as ordinal mRS, good functional outcome (mRS ≤2), excellent functional outcome (mRS ≤1), mRS shift analysis after 90 days, and early improvement of neurological findings at 48 hours. A total sample size of 200 was estimated to provide a power of 0.9 with a two-sided alpha of 0.05, for the primary outcome, considering a 15% dropout rate. This randomized clinical trial reported the applicability of endovascular therapy in patients with acute cerebral LVO with a large ischemic core.
- 著者
- Takahiro OTA Shogo DOFUKU Masayuki SATO
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.9, pp.69-72, 2022-12-31 (Released:2022-04-01)
- 参考文献数
- 11
- 被引用文献数
- 2
Posterior inferior cerebellar artery (PICA) variations are well recognized; however, their mechanisms have not been well understood. Primitive lateral basilovertebral anastomosis (PLBA) was described in 1948 by Padget and is one of the embryological transient longitudinal channels in the hindbrain. This study reports a PICA aneurysm associated with PLBA. A 48-year-old man presented with subarachnoid hemorrhage. Cerebral angiography showed a 3.6-mm fusiform aneurysm with a bleb of the left PICA just at the origin of the PICA from the vertebral artery. Furthermore, a direct anterior inferior cerebellar artery (AICA) -PICA anastomosis parallel to the basilar artery was revealed. This direct anastomosis between the AICA and PICA is explained by the partial persistence of PLBA. Variations in the three cerebellar arteries and vertebrobasilar junction can be caused by persistence of PLBA.
- 著者
- Mariko NODA Motoki INAJI Jun KARAKAMA Yukika ARAI Masae KUROHA Kaoru TAMURA Yoji TANAKA Taketoshi MAEHARA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.9, pp.13-17, 2022-12-31 (Released:2022-02-23)
- 参考文献数
- 23
- 被引用文献数
- 2
It has been reported that bevacizumab, an agent administered as an adjuvant therapy for high-grade gliomas, causes thromboembolic complications. We report a cerebral infarction with newly developed cerebral artery stenosis occurring during treatment with bevacizumab for an anaplastic astrocytoma. A 48-year-old female underwent excision surgery for an anaplastic astrocytoma on the right temporal lobe and received radiation therapy and chemotherapy with temozolomide. Twenty months after the maintenance therapy, treatment with bevacizumab was introduced for tumor recurrence. After the 14th course of bevacizumab at 6 months, 27 months after radiation therapy, the patient began experiencing mild right hemiparesis. Magnetic resonance imaging revealed scattered cerebral infarcts on the left frontal lobe and diffuse cerebral artery stenosis of the bilateral internal carotid artery system both inside and outside the radiation-treated area. Antiplatelet medication was commenced, and there was no recurrence of ischemic stroke. The morphological transition of the cerebral arteries should be carefully monitored via magnetic resonance angiography during post-radiation treatment with bevacizumab.
- 著者
- Toru YOSHIURA Satoru TAKEUCHI Terushige TOYOOKA Arata TOMIYAMA Kojiro WADA Yasuaki NAKAO Takuji YAMAMOTO Kentaro MORI
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- pp.2023-0157, (Released:2023-11-08)
- 参考文献数
- 28
In Japan, brain docking has enhanced the detection of unruptured intracranial aneurysms in healthy adults. At our institution, surgical clipping is the first-line treatment for unruptured intracranial aneurysms (UIA). In this study, the differences in neurological and radiological outcomes, as well as cognitive and psychological results, between standard clipping and keyhole clipping for these aneurysms detected via brain docking were evaluated. The study included 131 aneurysms detected via "brain dock." Of these, 65 were treated with keyhole clipping surgery (keyhole clipping group), and 66 were treated with standard clipping surgery (standard clipping group). Evaluations at 3 months included the National Institutes of Health Stroke Scale, modified Rankin Scale, Mini-Mental State Examination, Hasegawa's Dementia Scale-revised, Beck Depression Inventory, Hamilton Rating Scale for Depression, and radiological abnormalities. The mean operative time and postoperative hospitalization period were significantly shorter in the keyhole clipping group than in the standard clipping group (p < 0.001). Between the groups, no significant differences in postoperative neurological complications or radiological abnormalities were found. The keyhole clipping group demonstrated slightly but significantly better Beck Depression Inventory and Hamilton Rating Scale for Depression scores than the standard clipping group (Beck Depression Inventory, p = 0.046; Hamilton Rating Scale for Depression, p < 0.01). Both the Beck Depression Inventory and Hamilton Rating Scale for Depression scores at 3 months were significantly enhanced (p < 0.001) in the keyhole clipping group. These findings propose that keyhole clipping could be considered a new therapeutic option for small UIA detected via brain docking.
- 著者
- Ai NISHIYAMA Hidetaka WAKABAYASHI Shinta NISHIOKA Ayano NAGANO Ryo MOMOSAKI
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- pp.oa.2019-0002, (Released:2019-05-22)
- 参考文献数
- 23
- 被引用文献数
- 17
Our aim was to clarify the nutritional status and energy intake needed for activities of daily living (ADL) improvement among convalescent stroke patients. This retrospective cohort study of stroke patients used data from the Japan Rehabilitation Nutrition Database. Mean energy intake per ideal body weight was 26 kcal/kg/day at 1 week after hospitalization. Patients were divided into two groups according to energy intake: ≥26 kcal/kg/day (high) and <26 kcal/kg/day (low). ADL was evaluated using Functional Independence Measure (FIM), and nutritional status was evaluated using the mini nutritional assessment short form score. We created an inverse probability weighted (IPW) model using propensity scoring to control and adjust for patient characteristics and confounders at the time of admission. The analysis included 290 patients aged 78.1 ± 7.8 years. There were 165 patients with high energy intake and 125 patients with low energy intake. FIM score was significantly higher in the high group compared with the low group (median 113 vs 71, P <0.001). FIM efficiency was also higher in the high group (median 0.31 vs 0.22, P <0.001). FIM efficiency was significantly higher in the high energy intake group than in the low energy intake group after adjustment by IPW (median 0.31 vs 0.25, P = 0.011). Nutritional status improvement was also higher in the high energy intake group after adjustment by IPW (60.6% vs 45.2%, P <0.001). High energy intake was associated with higher FIM efficiency and nutritional status improvement at discharge among convalescent stroke patients.
- 著者
- Yoshimichi Sato Ryuta Saito Masayuki Kanamori Teiji Tominaga
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.7, no.1, pp.39-41, 2020 (Released:2020-01-01)
- 参考文献数
- 7
- 被引用文献数
- 3
Cystic tumors, such as craniopharyngiomas and Rathke’s cleft cysts, as well as arachnoid cysts have been reported to rupture occasionally. Approximately 8–10% of glioblastomas (GBMs) are known to have a significant cystic component; however, to the best of our knowledge, no studies have reported cystic rupturing of GBMs. Here, we describe a unique case of cystic GBM rupturing and penetrating into the cerebral ventricle. A 77-year-old man with a right frontal lobe lesion suspected as GBM with a large cyst was referred to our hospital. At admission, disorientation and left facial weakness were detected. Consciousness disturbance worsened on the 8th day of hospitalization. Computed tomography (CT) revealed prominent shrinkage of the tumor and intratumoral cyst. Signs of meningeal irritation were observed, and chemical meningitis due to cystic tumor rupture and leakage of necrotic components into the ventricle was highly suspected. Surgical resection of the right frontal lobe tumor was performed on the 10th day of hospitalization. During the surgery, clear and colorless cerebrospinal fluid was obtained upon penetration of the tumoral cyst, suggesting traffic of tumor cysts and cerebral ventricle. Adjuvant chemoradiation therapy was initiated postoperatively. Local recurrence was noted at the corpus callosum 7 months postoperatively and was treated with a gamma knife. Further therapy was performed after this recurrence. However, his condition gradually deteriorated 15 months postoperatively, and he was subjected to terminal care. To the best of our knowledge, this is the first report on a cystic GBM rupture.
- 著者
- Kyoko TATEBAYASHI Ichiro TAKUMI Takashi MATSUMORI Kimiyuki KAWAGUCHI Hidetoshi MURATA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.10, pp.321-325, 2023-12-31 (Released:2023-11-11)
- 参考文献数
- 23
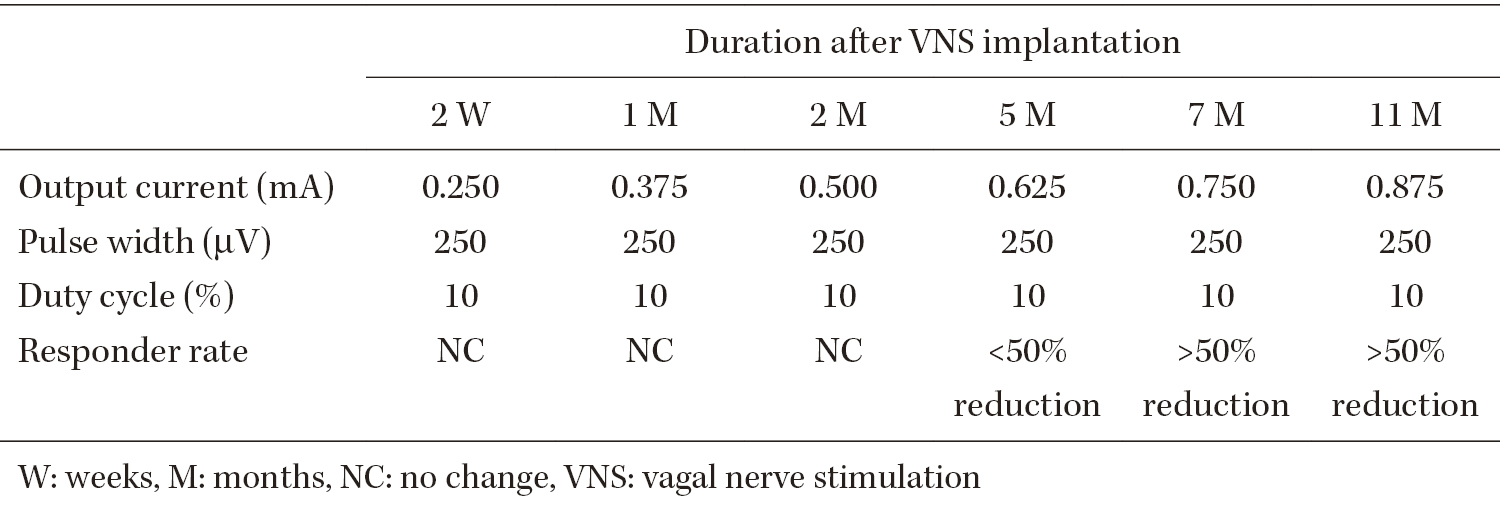
Epilepsy with eyelid myoclonia is a childhood-onset generalized epilepsy, which is more common in women. Over 90% of the patients continue antiseizure medications, especially valproate, and more than 60% of cases are refractory. The efficacy of vagus nerve stimulation in treating eyelid myoclonia is still unknown. Polycystic ovary syndrome is highly prevalent in women with epilepsy receiving valproate; nevertheless, no reports on the complication of polycystic ovary syndrome in women with epilepsy with eyelid myoclonia were found. In this report, a case of a woman with epilepsy with eyelid myoclonia who developed polycystic ovary syndrome while receiving valproate and underwent vagus nerve stimulation is described. A 26-year-old female patient has been administered valproate since the occurrence of generalized seizures at the age of 12 years and then developed polycystic ovary syndrome. When the dose of valproate was reduced as an adult, her epilepsy became intractable. Information from her mother led to a video electroencephalography re-evaluation, and she was finally diagnosed 15 years after onset. The patient underwent vagus nerve stimulation. In a short-term follow-up, she achieved >50% seizure reduction at low output currents of <1.00 mA. Polycystic ovary syndrome was cured 15 months after valproate withdrawal. There are three key points presented in this case: Vagus nerve stimulation therapy was useful for treating epilepsy with eyelid myoclonia with absence. Women with epilepsy with eyelid myoclonia taking valproate must be aware of the risk of polycystic ovary syndrome and monitor their menstrual cycles. Information from the family, such as home videos, helped with the diagnosis.
- 著者
- Kentaro CHIBA Yasuo AIHARA Yuichi ODA Kenta MASUI Takashi KOMORI Hideaki YOKOO Takakazu KAWAMATA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.10, pp.265-271, 2023-12-31 (Released:2023-10-14)
- 参考文献数
- 32
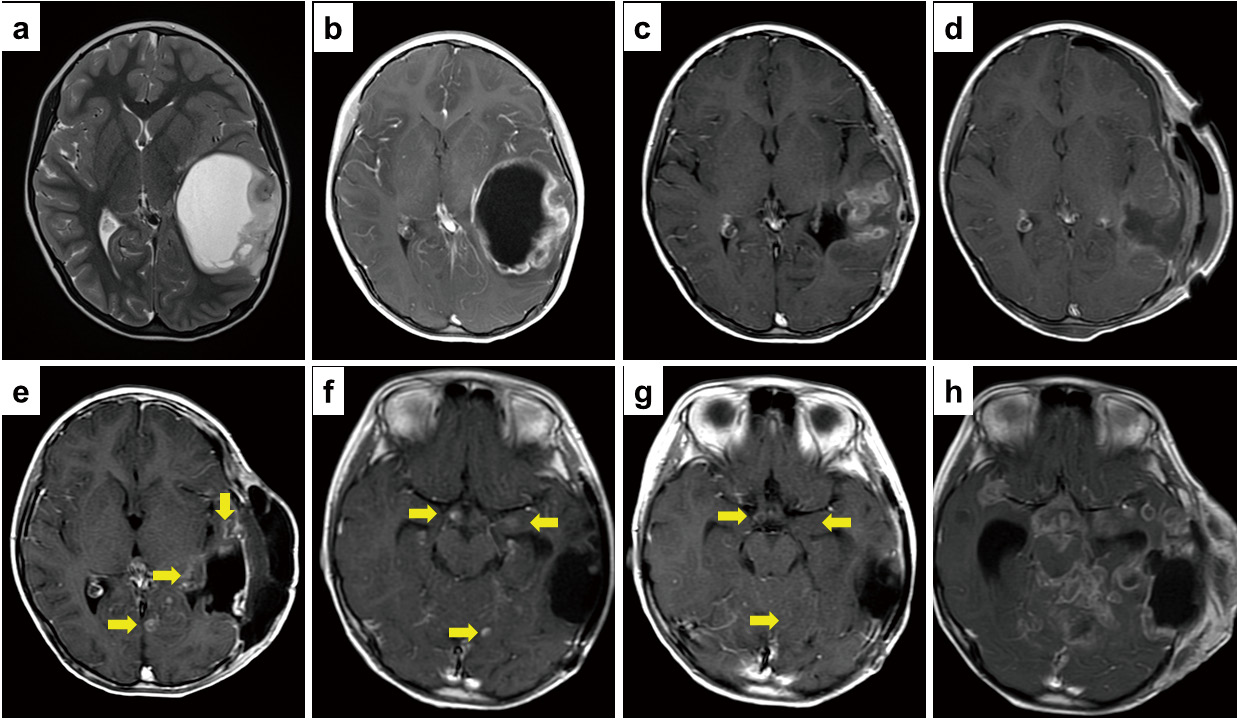
Extracranial brain tumor metastases are extremely rare. The etiology, pathophysiology, and clinical progression of systemic metastatic brain cancer remain to be elucidated. We encountered a case of pediatric diffuse high-grade astrocytoma in a four-year-old girl with subcutaneous and lymph node metastases. Numerous metastatic lesions emerged, progressed rapidly, and were difficult to manage despite temozolomide (TMZ) administration. The patient underwent repeated surgical resection for these lesions. Conversely, the primary intracranial lesions responded well to TMZ for some time. However, the patient died 15 months after the initial diagnosis. Extracranial metastasis and highly varying effects of chemotherapy were the characteristic clinical features in this case. Our analysis did not reveal definitive histopathological and molecular factors contributing to this presentation. The lack of notable molecular pathological features illustrates the unpredictability of glioma metastasis, and the treatment for extracranial metastasis remains unknown. A gene panel analysis revealed several genetic aberrations, including PDGFRA, PIK3CA, and NBN mutations. As it is impossible to resect all frequently and rapidly progressing lesions, we stress that the prognosis of metastatic brain tumors is undoubtedly poor if these tumors are refractory to existing treatments, including chemotherapy.
- 著者
- Yutaro TAKAYAMA Kazutaka JIN Shin-ichiro OSAWA Masaki IWASAKI Kazushi UKISHIRO Yosuke KAKISAKA Teiji TOMINAGA Tetsuya YAMAMOTO Nobukazu NAKASATO
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.8, no.1, pp.773-780, 2021 (Released:2021-11-02)
- 参考文献数
- 32
Cognitive decline is a well-known chronic side effect of multidisciplinary treatment of pineal region tumors, whereas epilepsy is an under-reported chronic consequence caused by multiple potential factors including radiotherapy, surgery, or chemotherapy. Some long-term survivors have suffered drug-resistant epilepsy after treatment, which impaired the quality of life. We report five consecutive patients with drug-resistant epilepsy after combined treatment of pineal region tumor (5 men, aged 21–42 years) among 1201 epilepsy patients who underwent comprehensive evaluation in our tertiary epilepsy center from 2011 to 2018. The comprehensive epilepsy evaluation included medical interview, long-term video electroencephalography (EEG) monitoring (VEM), and magnetic resonance (MR) imaging. The patients started to have seizures at 2–22 years after initial treatment for the tumor. Four of the five patients had focal impaired awareness seizures, whereas one patient had only visual aura. All patients had EEG seizures during VEM, which confirmed the diagnosis of focal epilepsy, but three patients had no interictal epileptiform discharges (IEDs). Two patients had diagnoses of focal epilepsy arising from the left occipital region based on ictal EEG findings. Both patients had MR imaging lesion in the left occipital lobe, radiation-induced cavernoma, or surgical injury. The remaining three patients showed poor localization of epileptogenic foci based on VEM and MR imaging. Drug-resistant epilepsy after multidisciplinary treatment of pineal region tumor is characterized by focal impaired awareness seizures with poorly localized EEG onset or rare interictal spikes.
- 著者
- Madoka NAKAJIMA Shigeki YAMADA Masakazu MIYAJIMA Kazunari ISHII Nagato KURIYAMA Hiroaki KAZUI Hideki KANEMOTO Takashi SUEHIRO Kenji YOSHIYAMA Masahiro KAMEDA Yoshinaga KAJIMOTO Mitsuhito MASE Hisayuki MURAI Daisuke KITA Teruo KIMURA Naoyuki SAMEJIMA Takahiko TOKUDA Mitsunobu KAIJIMA Chihiro AKIBA Kaito KAWAMURA Masamichi ATSUCHI Yoshihumi HIRATA Mitsunori MATSUMAE Makoto SASAKI Fumio YAMASHITA Shigeki AOKI Ryusuke IRIE Hiroji MIYAKE Takeo KATO Etsuro MORI Masatsune ISHIKAWA Isao DATE Hajime ARAI The research committee of idiopathic normal pressure hydrocephalus
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- vol.61, no.2, pp.63-97, 2021 (Released:2021-02-15)
- 参考文献数
- 286
- 被引用文献数
- 88 211
Among the various disorders that manifest with gait disturbance, cognitive impairment, and urinary incontinence in the elderly population, idiopathic normal pressure hydrocephalus (iNPH) is becoming of great importance. The first edition of these guidelines for management of iNPH was published in 2004, and the second edition in 2012, to provide a series of timely, evidence-based recommendations related to iNPH. Since the last edition, clinical awareness of iNPH has risen dramatically, and clinical and basic research efforts on iNPH have increased significantly. This third edition of the guidelines was made to share these ideas with the international community and to promote international research on iNPH. The revision of the guidelines was undertaken by a multidisciplinary expert working group of the Japanese Society of Normal Pressure Hydrocephalus in conjunction with the Japanese Ministry of Health, Labour and Welfare research project. This revision proposes a new classification for NPH. The category of iNPH is clearly distinguished from NPH with congenital/developmental and acquired etiologies. Additionally, the essential role of disproportionately enlarged subarachnoid-space hydrocephalus (DESH) in the imaging diagnosis and decision for further management of iNPH is discussed in this edition. We created an algorithm for diagnosis and decision for shunt management. Diagnosis by biomarkers that distinguish prognosis has been also initiated. Therefore, diagnosis and treatment of iNPH have entered a new phase. We hope that this third edition of the guidelines will help patients, their families, and healthcare professionals involved in treating iNPH.
- 著者
- Takamasa KINOSHITA Hirohito YANO Noriyuki NAKAYAMA Natsuko SUZUI Tomohiro IIDA Saori ENDO Shiho YASUE Michio OZEKI Kazuhiro KOBAYASHI Tatsuhiko MIYAZAKI Toru IWAMA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.8, no.1, pp.151-157, 2021 (Released:2021-06-05)
- 参考文献数
- 43
Giant cell glioblastoma (GCG) is a rare subtype of glioblastoma multiforme (GBM), and it often occurs in younger patients; however, its onset in children is extremely noticeable. A 7-year-old girl presented with a headache and restlessness. A giant tumor that was 7 cm in diameter was found by magnetic resonance imaging (MRI) in the left frontal lobe with intracranial dissemination. Because the tumor had extended to the lateral ventricles and occluded the foramen of Monro causing hydrocephalus, she underwent ventricular drainage and neuro-endoscopic biopsy from the left posterior horn of the lateral ventricle. The initial pathological diagnosis was an atypical teratoid/rhabdoid tumor (AT/RT). When the dissemination subsided after the first chemotherapy with vincristine, doxorubicin, and cyclophosphamide, she underwent the first tumor resection via a left frontal transcortical approach. After surgery, the second chemotherapy with ifosfamide, cisplatin, and etoposide was not effective for the residual tumor and intracranial dissemination. The second surgery via a transcallosal approach achieved nearly total resection leading to an improvement of the hydrocephalus. The definitive pathological diagnosis was GCG. Despite chemo-radiation therapy, the dissemination in the basal cistern reappeared and the hydrocephalus worsened. She was obliged to receive a ventriculo-peritoneal (VP) shunt and palliative care at home; however, her poor condition prevented her discharge. Ten months after admission, she died of tumor progression. The peritoneal dissemination was demonstrated by cytology of ascites. In conclusion, although unusual, pediatric GCG may be disseminated at diagnosis, in which case both tumor and hydrocephalus control need to be considered.
6 0 0 0 OA Radiofrequency Ventro-oral Thalamotomy for Post-stroke Focal Dystonia in a Pediatric Patient
- 著者
- Noriko HIRAO Takashi MORISHITA Kazuya SAITA Tomohiro TAKAGI Shinsuke FUJIOKA Tooru INOUE
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.8, no.1, pp.445-450, 2021 (Released:2021-08-06)
- 参考文献数
- 15
Dystonia is a movement disorder that has various treatment options. For primary dystonia, stereotactic procedures such as deep brain stimulation (DBS) have demonstrated favorable outcomes. For secondary dystonia, however, the treatment outcomes remain inconclusive, and the heterogeneous etiological background is considered to contribute to the poor outcomes of the disease. Here, we report a rare pediatric case of post-stroke focal dystonia treated with conventional radiofrequency ventro-oral (Vo) thalamotomy. The patient was an 11-year-old girl with secondary focal dystonia in her right hand. The dystonia was considered to result from a stroke lesion in the putamen due to vasculitis following varicella-zoster virus infection. We hypothesized that the infarction of the putamen resulted in hyperactivity in the thalamus, and, thus, performed a radiofrequency Vo thalamotomy. Markedly decreased muscle tone in her right hand was noted immediately after surgery. However, the improvement was temporary, as her symptoms returned to baseline level by the 6-month follow-up. Although the observed improvement was temporary in this case, our findings may elucidate the possible mechanisms of secondary focal dystonia. Further studies are needed to establish an effective surgical treatment for secondary focal dystonia.
- 著者
- Etsuro MORI Masatsune ISHIKAWA Takeo KATO Hiroaki KAZUI Hiroji MIYAKE Masakazu MIYAJIMA Madoka NAKAJIMA Masaaki HASHIMOTO Nagato KURIYAMA Takahiko TOKUDA Kazunari ISHII Mitsunobu KAIJIMA Yoshihumi HIRATA Makoto SAITO Hajime ARAI
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- vol.52, no.11, pp.775-809, 2012 (Released:2012-11-25)
- 参考文献数
- 253
- 被引用文献数
- 149 480
Among the various disorders manifesting dementia, gait disturbance, and urinary incontinence in the elderly population, idiopathic normal pressure hydrocephalus (iNPH) is becoming of great importance. After the publication of the first edition of the Guidelines for Management of Idiopathic Normal Pressure Hydrocephalus in 2004 (the English version was published in 2008), clinical awareness of iNPH has risen dramatically, and the number of shunt surgeries has increased rapidly across Japan. Clinical and basic research on iNPH has increased significantly, and more high-level evidence has since been generated. The second edition of the Japanese Guidelines was thus published in July 2011, to provide a series of timely evidence-based recommendations related to iNPH. The revision of the Guidelines has been undertaken by a multidisciplinary expert working group of the Japanese Society of Normal Pressure Hydrocephalus in conjunction with the Japanese Ministry of Health, Labour and Welfare research project on “Studies on the epidemiology, pathophysiology, and treatment of normal pressure hydrocephalus.” This English version of the second edition of the Guidelines was made to share these ideas with the international community and to promote international research on iNPH.
- 著者
- Ayaka SASAGAWA Takeshi MIKAMI Yusuke KIMURA Yukinori AKIYAMA Shintaro SUGITA Tadashi HASEGAWA Masahiko WANIBUCHI Nobuhiro MIKUNI
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- pp.oa.2020-0309, (Released:2020-12-29)
- 参考文献数
- 23
- 被引用文献数
- 2
Gliomas are sometimes difficult to differentiate from strokes and are often misdiagnosed on magnetic resonance imaging (MRI); thus, the terms “stroke mimics” and “stroke chameleons” have been introduced. In this study, we analyzed stroke mimics and stroke chameleons in glioma and discussed the diagnostic perplexity.We retrospectively reviewed cases that were removed from lesions that were considered to be brain tumors. This study enrolled 214 patients who underwent tumor resection for suspected glioma. Clinical characteristics and radiological findings of the patients were compared between the masquerade findings group, which was further divided into two groups: the stroke chameleons and stroke mimics according to their final diagnosis, and the intelligible findings group.Stroke chameleons and stroke mimics were significantly higher in age and smaller in lesion size than the intelligible findings group. In the multivariate analysis, the predictive factor of the masquerade finding group was higher age and smaller size. Stroke mimics group has a tendency to be higher rate of hyperintensity lesion on diffusion-weighted imaging (DWI) compared with stroke chameleons group. The average period from initial diagnosis to pathological diagnosis was 13.50 days in the stroke chameleons and 61.50 days in the stroke mimics, which proved significantly different.Proper diagnosis of glioma and stroke affects a patient’s prognosis, and should be diagnosed as soon as possible. However, stroke mimics and stroke chameleons caused by glioma can occur. Thus, the diagnosis of a stroke should take into consideration the possibility of a glioma in real clinical situations.
- 著者
- Shota YAMASHITA Ryuta SAITO Shin-ichiro OSAWA Kuniyasu NIIZUMA Kazushi UKISHIRO Masayuki KANAMORI Kazuo KAKINUMA Kyoko SUZUKI Teiji TOMINAGA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- Neurologia medico-chirurgica (ISSN:04708105)
- 巻号頁・発行日
- vol.61, no.11, pp.661-666, 2021 (Released:2021-11-15)
- 参考文献数
- 21
- 被引用文献数
- 3
In cases of malignant gliomas located at language eloquent area, it is often difficult to preoperatively detect those area with functional MRI. Awake surgery is often used to spare the language eloquent area during surgery for such tumors; it is not available for a patient whose intracranial pressure is elevated due to the malignant tumor. The Wada test involves infusing anesthetic agents into the internal carotid artery to determine language dominancy before surgery for epilepsy or brain tumor. The super-selective Wada test is a technique to detect more detailed functional localization by infusing anesthetics into far distal middle cerebral artery branches. We present a 37-year-old man suffering from a left frontal lobe glioblastoma, in whom detection of an artery supplying Broca’s area was attempted by a super-selective Wada test. The super-selective Wada test successfully detected the branch of middle cerebral artery supplying Broca’s area. Total resection of the contrast-enhancing area was achieved without damaging the artery supplying Broca’s area without any neurological sequelae. This is the first report describing the usefulness of the super-selective Wada test in glioblastoma treatment. Our findings suggest that the super-selective Wada test is a powerful and useful means to distinguish the artery that supplies the language area from the tumor feeding artery in cases of tumors in the language eloquent area.
- 著者
- Novita Ikbar KHAIRUNNISA Fumiyuki YAMASAKI Vishwa Jeet AMATYA Takeshi TAKAYASU Ushio YONEZAWA Akira TAGUCHI Shumpei ONISHI Nobutaka HORIE
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.9, pp.395-400, 2022-12-31 (Released:2022-11-15)
- 参考文献数
- 22
Temozolomide is an oral alkylating agent with moderate side effects compared to other agents. However, the development of secondary malignancies following temozolomide has been reported. We describe the first case of primary central nervous system lymphoma (PCNSL) occurrence following glioblastoma treatment. A 69-year-old male was admitted to our hospital with a chief complaint of headache and dysnomia for six months. A ring-enhanced mass of the left temporal lobe was observed and gross total removal was performed. The tumor was pathologically diagnosed as isocitrate dehydrogenase (IDH) -wildtype glioblastoma and he received 60 Gy of local irradiation in 30 fractions, with concurrent temozolomide at a dose of 75 mg/m2. Grade 2 lymphopenia was discovered during treatment. Within 6 months, the patient developed a right parietal intra-axial tumor without local recurrence and was given 150-200 mg/m2 oral temozolomide for five consecutive days of a 28-day cycle. Within five cycles of temozolomide, complete remission was observed; however, after the eighth cycle, a new lesion in the right temporal lobe was discovered. Surgical removal was performed and histological findings were consistent with diffuse large B-cell lymphoma, and the final diagnosis of Epstein-Barr virus negative PCNSL was established.
- 著者
- Takaharu KAWAJIRI Hayato TAKEUCHI Yoshinobu TAKAHASHI Yuji SHIMURA Junya KURODA Naoya HASHIMOTO
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.10, pp.131-137, 2023-12-31 (Released:2023-05-17)
- 参考文献数
- 22
Eating disorders caused by brain tumors are infrequently seen. Recent studies revealed that a neurocircuit from the nucleus tractus solitarius of the medulla oblongata to the hypothalamus participates in the control of appetite. Among brain tumors, those located in the brain stem, especially a solitary one in the medulla oblongata, are rare. Tumors in the brainstem are generally considered gliomas, and with the difficulty in reaching the lesion, treatment without histological confirmation is often performed. However, there are a few reported cases of medulla oblongata tumors other than gliomas. We describe a case of a 56-year-old man who presented with persistent anorexia. Magnetic resonance images revealed a solitary tumor in the medulla oblongata. After several examinations, craniotomy for the biopsy of the tumor using the cerebellomedullary fissure approach was carried out and primary central nervous system lymphoma (PCNSL) was histologically proven. The patient was treated with effective adjuvant therapy and was discharged home after he recovered from the symptoms. No tumor recurrence was recognized 24 months after surgery. A PCNSL arising only from the medulla oblongata is very rare, and anorexia can be an initial symptom of a tumor in the medulla oblongata. Surgical intervention is safely achieved and is a key to a better clinical outcome.
- 著者
- Yuki HAMADA Fumio MIYASHITA Hideki MATSUOKA Yuki NISHINAKAMA Yusuke KAI Yusuke YAMASHITA Mei IKEDA Go TAKAGUCHI Keisuke MASUDA Fumikatsu KUBO Hiroshi TAKASHIMA
- 出版者
- The Japan Neurosurgical Society
- 雑誌
- NMC Case Report Journal (ISSN:21884226)
- 巻号頁・発行日
- vol.10, pp.273-278, 2023-12-31 (Released:2023-10-14)
- 参考文献数
- 12
Herein, we report a case of carotid artery stenting with proximal flow protection for severe stenosis of the left internal carotid artery using transbrachial and transradial artery approaches. Because an abdominal aortic aneurysm was present, we avoided the transfemoral approach. The procedure was successfully performed with a combination of an 8-Fr balloon guide catheter and microballoon catheter on separate axes. No complications such as pseudoaneurysm, thrombosis, or dissection were observed at the puncture site. The patient was discharged without complications and showed good outcomes at 3 months. This technique may offer a useful alternative for patients with severe stenosis who cannot be treated using a femoral artery approach.